Trends in Animal Antibiotic Use - Europe
There is good reason to be concerned about the overuse of antibiotics in both humans and animals. As the animal health sector we have been promoting the ‘responsible use’ of veterinary antibiotics since 2005 through our European Platform for Responsible Use of Medicines in Animals. Antibiotic resistance is a recognised global One Health challenge and we must all do what we can to help preserve the effectiveness of antibiotics for both people and animals.
Antibiotics are a cornerstone of modern medicine and will remain essential tools to treat bacterial diseases; there are currently no alternatives. Their importance to human and animal health cannot be understated, which is why the animal health sector must be part of the solution and has been at the forefront of efforts to promote responsible use and preserve their efficacy.
This paper analyses key data to understand how efforts are progressing in Europe, and how we can better understand and tackle AMR in a One Health manner.
1. Animal antibiotic use is falling: In Europe antibiotic sales have fallen by 53% since 2011.
2. Prevention works: Rises in sales of prevention products appear to be mirrored by reductions in sales of antibiotics.
3. Antibiotics remain a critical tool: Many countries have achieved large declines in sales that eventually plateau or level off. This may reflect a state of ‘optimal use’ where prevention and other measures such as biosecurity are optimised, but antibiotics remain necessary for treatment of disease that evades a farm’s defences.
4. Progress cannot be achieved without One Health action: Authorities like the ECDC have found that the majority of human AMR transfer stems from human health care settings. Research indicates actions within the animal domain, without corresponding action in human health, will have little impact on the overall burden of antibiotic resistance in human health.
5. Animal health is taking a leading role: Authorities have recognised the significant progress made in reducing the need for antibiotics in animals.
Animal antibiotic use has fallen across Europe
Global antimicrobial use is also declining
The World Organisation for Animal Health (WOAH) collects global antimicrobial use data from 120+ countries worldwide. WOAH reported in their 2023 annual summary that “global antimicrobial use in animals has declined by 13% between 2017-2019”.
Sources: European Medicines Agency, World Organisation for Animal Health, Annual report on Antimicrobial Agents Intended for Use in Animals, 7th Edition
Antimicrobial sales have fallen more than 50% in major livestock-producing countries across Europe
Decreases measured in mg/PCU as defined by EMA (except UK in mg/Kg).
Although sales can offer an indicator of trends in antimicrobial use, it cannot measure whether AMR is rising or falling. Only testing for resistance itself can achieve this, which is why sales reporting must be accompanied by AMR surveillance.
Sources: UK Veterinary Medicines Directorate, ESVAC Italy trends report, ESVAC France trends report, ESVAC Germany trends report, ESVAC Netherlands trends report, ESVAC Spain trends report
Large reductions are reported for EMA priority veterinary antimicrobial classes*
Using these shared class products only when necessary, can help limit cross resistance development.
*AMEG category B: EMA/AMEG 2019, Categorisation of antibiotics in the European Union
There is limited veterinary use of priority antimicrobial classes
There is limited or no veterinary use of the most important human antimicrobials. Very rarely some may need to be used to treat specific bacterial infections in animals, for which there is no alternative treatment: many cannot be used in animals at all.
Sales of antimicrobial active substances by antimicrobial class as percentages of the total sales
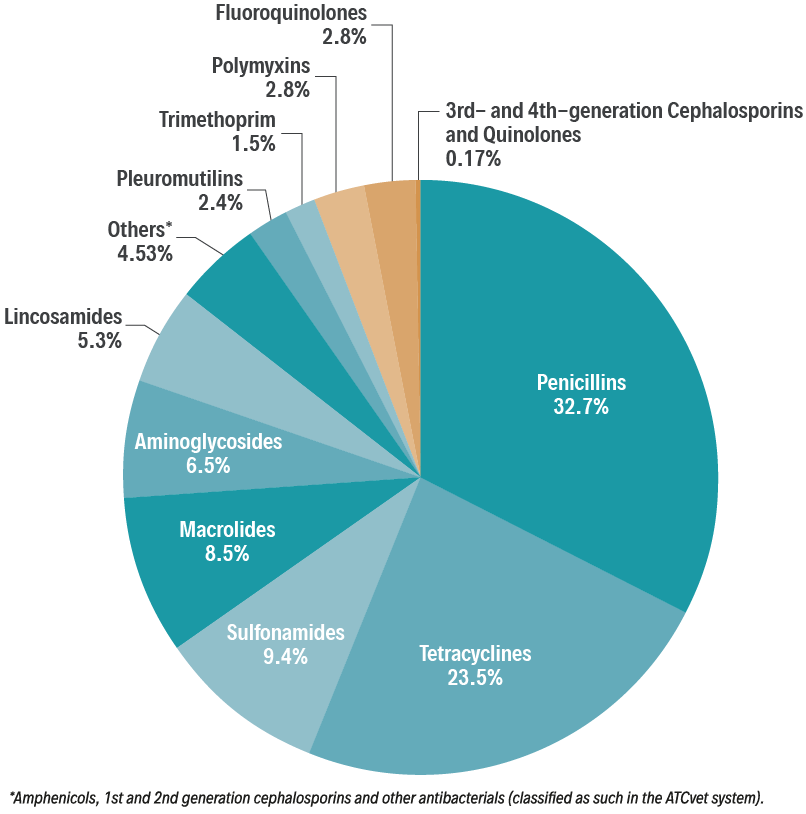
Classed as medically important by Antimicrobial Advice Ad Hoc Expert Group (AMEG) and adopted by both EMA’s veterinary medicines committee (CVMP) and human medicines committee (CHMP)
Source: European Medicines Agency
Sales of prevention products are increasing which can reduce the need for antibiotics
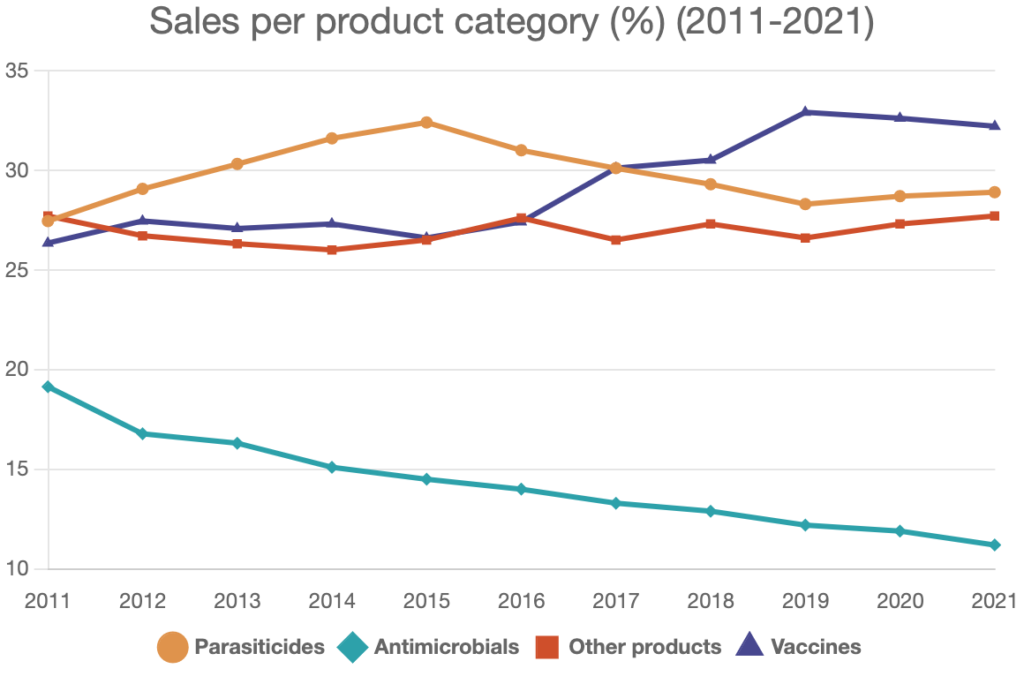
Sales data from leading animal health companies demonstrate how the increased focus on prevention is reducing the need for antimicrobials. Since 2011, sales of vaccines and parasiticides combined have grown from 53.8% to 61.1% of the product portfolio while antimicrobials fell from 19.4% to 11.2% (a relative reduction of around 42%).
Source: Executive Animal Health Study Centre CEESA
Many countries are achieving steady optimal levels of use
Animal antimicrobial sales trends (2010–2020)
Steep declines in antimicrobial sales levelling off to a consistent level may reflect a state of ‘optimal use’ where prevention is optimised, but antibiotics remain necessary for treatment of disease that evades a farm’s defences. This serves as a reminder that not all illness can be prevented, and these medicines remain the only way to treat bacterial disease.
The below charts demonstrate how animal antimicrobial sales have changed over the past decade for four nations. Sales levels differ for each (see source for underlying numbers), however the trend lines are similar for all.
Source: European Medicines Agency
Denmark
France
Netherlands
United Kingdom
*population correction unit
One Health action is necessary for minimising development of AMR
AMR is a One Health challenge
Addressing development of antimicrobial resistance requires complementary action across human health, animal health and environmental sectors. This means reducing the need for antibiotics, researching transfer pathways, and strengthening surveillance across all three domains.
A University of Edinburgh study suggested that reducing antibiotic use only in animals but not in people has “little impact on the level of resistance in humans.”
Source: Royal Society Open Science
“More progress in agriculture than in the human sector”
A report on antimicrobial resistance from the European Medicines Agency (EMA), European Food Safety Authority (EFSA), European Centre for Disease Control (ECDC) and OECD found there was “more progress in agriculture than in the human sector” and since 2016, “average consumption of antibiotics in humans is now higher than in food-producing animals”. However, some markets have decreased human consumption of antibiotics alongside animal reductions. The report found that overall human antibiotic use in the EU had fallen, although when looking at specific classes, broad-spectrum antibiotic use in humans was still rising.
Source: Antimicrobial Resistance in the EU/EEA: A One Health Response
Comparing use levels between people and animals
Developing a clear, reliable comparison between antimicrobial use in humans and animals is challenging. 1-to-1 comparison in volumes used is often misleading since a beef cattle weighing over 500 kilos will naturally require a different type and dosage of medicine compared to a 70 kg person. Therefore, when comparing quantities, it is important to consider:
- There are many more animals than humans, and there are differences in physiology and weight between humans and animals.
- Different species metabolise antimicrobials differently, meaning that some species may require more in volume to be effective, or may need to be treated for a longer period.
- Different antibiotics have different potencies. Older antibiotics such as tetracyclines – one of the largest groups used in animal care – tend to have much higher doses than newer antibiotics such as fluoroquinolones.
Global authorities such as the World Organisation for Animal Health (WOAH) and leading markets have developed systems to measure the amount of antibiotics used per kilogramme of biomass. These provide a greater standardisation that better illustrates trends in antibiotic use and enables comparisons.
Understanding pathways for AMR development and transfer
Researchers from leading institutions have undertaken robust analysis to better understand how AMR develops and transfers between people and across species. This essential work helps with better targeting efforts to minimise the development of resistance.
Potential actions for tackling AMR are endless, but funding, time and manpower are not. This is why public authorities and European and international institutions have invested in better understanding where AMR transfer occurs, what actions can be most effective, and when it may originate in animals. Strategies must focus on actions that provide the greatest potential impact.
Potential actions for tackling AMR are endless, but funding, time and manpower are not. Strategies must focus on actions that provide the greatest potential impact. This is why public authorities and international institutions have invested in better understanding where AMR transfer occurs, what actions can be most effective, and when it may originate in animals.

In a landmark study, the European Centre for Disease Prevention and Control found that “75% of disease linked to resistant bacteria is due to healthcare-associated infections”
Source: ECDC

An OECD analysis of antimicrobial resistance found that “three out of four deaths could be averted by spending just USD 2 per person a year on measures as simple as handwashing and more prudent prescription of antibiotics”
Source: OECD
The UK Government in a five-year antimicrobial strategy reported that “Increasing scientific evidence suggests that the clinical issues with antimicrobial resistance that we face in human medicine are primarily the result of antibiotic use in people, rather than the use of antibiotics in animals”
Source: UK Department of Health & DEFRA
Together, these reports indicate that animals can play a role in AMR development in humans, which is why the stewardship and progress outlined in this report is so critical, but complementary action in human health is needed to make significant gains in the years ahead.
AMR can only be managed through a One Health approach that works across human, animal and environmental health.
Animal health sector taking a leading role
Coordinated action
AnimalhealthEurope together with the Federation of Veterinarians of Europe (FVE) and the European farmers and agri-cooperatives association (Copa Cogeca) had the foresight to create a multi-stakeholder platform back in 2005 to ensure coordinated action in addressing AMR. The European Platform for Responsible Use of Medicines in Animals (EPRUMA) was inspired from the UK’s Responsible Use of Medicines in Agriculture Alliance, and they have been working together for over almost two decades to improve animal health and ensure responsible use of antimicrobials, a unique approach not yet replicated in human health.
Today EPRUMA partners also work with national platforms in Belgium, the Netherlands, Spain and the UK to ensure tailored approaches for different countries.






Data Collection
All AnimalhealthEurope member companies have been providing antimicrobial sales data to the European Medicines Agency’s ESVAC report since it first started collecting data in 2010.
Reporting will be further improved thanks to updates from the 2019 EU Regulation on Veterinary Medicines which makes reporting by Member States on the volume of sales and the use of antimicrobials per animal species and per types of antimicrobial medicinal product mandatory.

International institutions are also stepping up efforts to improve data collection on antimicrobial use worldwide. The World Organisation for Animal Health’s Annual Report on Antimicrobial Agents Intended for Use in Animals provides invaluable data that is helping to better target efforts.
Clear Commitments
Our global association HealthforAnimals, with whom we share many member companies, launched a ‘Roadmap to Reducing the Need for Antibiotics in Animals’ in 2019 outlining a list of 25 measurable actions the animal health sector aims to complete by 2025. The Roadmap also offers a vision for improving responsible use and preventing disease.


Measurable Outcomes
In 2023, the global animal health sector released a second Roadmap Progress Report showing that all 25 commitments made in the Roadmap were on track for completion. This included delivering 71 new vaccines, training 1.77 million veterinary professionals and donating nearly over $15 million in veterinary scholarships in four years.
Altogether, these actions show that the animal health sector is taking a leading role in tackling antimicrobial resistance and our strong, collective action will continue in the coming years.
However, AMR cannot be overcome alone. Animal health companies and organisations remain committed to work together and share our knowledge and best practices to help strengthen the actions of others for our collective One Health.

